Airway Center
Complex Airway Center
Complex airway diseases are comprised of cancerous and non-cancerous disorders of the windpipes affecting breathing and speech. They develop in the larynx, trachea and mainstem bronchi, the windpipes that travel from the larynx to the lungs. Airway diseases can appear in many forms and are often misdiagnosed as other lung problems such as asthma, emphysema or chronic bronchitis.
Cancers affecting the windpipes include tumors of the larynx, thyroid, lung or can be caused by tumors from other organs such as the breasts, kidney, colon and skin. Non-cancerous disorders are mainly caused by prolonged intubation, tracheostomy or auto-immune disorders, but often there is no cause.
These disorders are complex due to the need for comprehensive evaluation and specialized procedures offered by a multidisciplinary team. Our team consists of thoracic surgeons, ear nose and throat (ENT) surgeons and interventional pulmonologists.
Symptoms
The symptoms of complex airway diseases will vary from person to person, but the most common symptoms are:
- Shortness of breath, especially with exertion or exercise, but can be present at rest when severe
- Cough, sometimes described as a “seal barking cough”
- Hoarseness
- Chest congestion, with inability to clear mucus
- Wheeze, a sound that occurs as you breathe out
- Stridor, a high-pitched sound that occurs as you breathe in or out
Although rapid worsening can happen, symptoms from complex airway diseases usually progress slowly and gradually worsen over time. Because these symptoms may resemble other lung conditions or medical problems, an accurate diagnosis is essential to ensure proper treatment. Patients should seek medical attention when they are known to have a narrowing of the windpipe or when they develop worsening symptoms such as, shortness of breath, voice changes, wheezing or coughing up blood.
Types of Complex Airway Diseases
Airway trauma can occur in several ways:
- Tracheal laceration after intubation
- Trachea-esophageal fistula, an abnormal connection in one or more places between the trachea and esophagus
- Persistent tracheal stoma that develops when a tracheostomy site does not heal
Bronchial stenosis is the narrowing of the bronchial tubes, which are the tubes that allow air in and out of the lungs. It can be caused by a variety of cancers, but it’s also seen in patients suffering from autoimmune disorders, post lung transplant, post radiation therapy or prior infections.
Similar to tracheobronchomalacia but much more common, excessive dynamic airway collapse occurs when the airway narrows after significant collapse of the posterior tracheal and bronchial membranous walls. This is typical in patients suffering from emphysema and obesity.
The glottis, the space between the vocal cords, is important in speech and breathing. Glottic stenosis is a condition where the space between the vocal cords is narrowed. This may cause issues with not only breathing, but also hoarseness and voice change. Additionally, swallowing problems may accompany this disorder. This problem may be caused by trauma to the larynx or after radiation therapy.
Tracheobronchomalacia refers to the weakness of the airway cartilaginous structures, causing it to collapse when breathing. It can be caused by autoimmune and connective tissue disorders, such as relapsing polychondritis or Ehlers-Danlos syndrome.
Tracheal tumors are rare and can be benign or malignant. Malignant tracheal cancers include adenoid cystic carcinoma, squamous cell carcinoma and carcinoid tumors. Often, patients will have symptoms for a long time and see many doctors before receiving a diagnosis. This is because tracheal tumors are difficult to diagnose and symptoms are often attributed to more common disorders such as asthma. The diagnosis is usually made by a dedicated neck or chest CT scan and bronchoscopy.
Bronchial tumors can be benign, but are often due to lung cancer or tumoral deposits from other cancers, including lymphoma, melanoma, breast, colon and kidney cancers.
Tracheal and subglottic stenosis is the narrowing of the trachea or the larynx, causing breathing problems. Most often, tracheal stenosis occurs when scar tissue forms in your trachea due to intubation or prior tracheostomy. Sometimes, prior airway infections such as tuberculosis, can lead to stenosis, or it can occur without a cause at all.
Subglottic stenosis can occur without a clear cause, but can be been seen in patients diagnosed with granulomatosis with polyangiitis (GPA) or relapsing polychondritis.
Treatment Options
Whether you are experiencing worsening symptoms or seeking a second opinion, our team of airway experts from interventional pulmonology, otolaryngology and thoracic surgery collaborate to provide specialized care for complex airway diseases. Through this team-based approach, our specialists can develop a personalized care plan, and if necessary, perform surgical repair.
At the University of Chicago Medicine, our experts perform innovative techniques with exceptional skill and excellent outcomes to treat complex airway diseases, including:
- Dilation
- Stenting
- Laser therapy
- Light therapy
- Ablation therapy
- Steroid injections
- Surgery
This technique stretches the airway to improve airway size and reduces symptoms. Bronchoscopic or laryngoscopic dilatations are often performed in combination with laser treatments of the airway scar tissue or tumor. Sometimes, insertion of dedicated airway stents is needed to maintain the airways opened.
During airway stenting, a tube is inserted to maintain an open airway. Stents are either silastic or metallic depending on if the stenosis is benign or malignant, the shape and location of the airway narrowing.
Metallic Airway Stent Procedure Photos
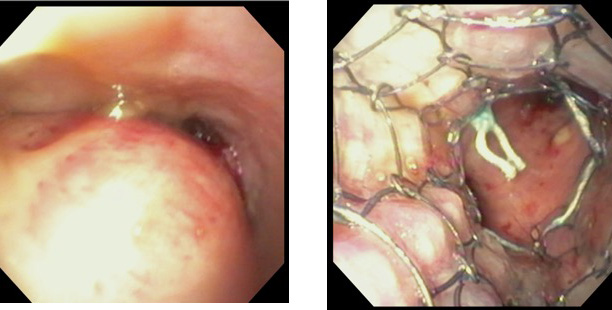
Silicone Airway Stent Procedure Photos
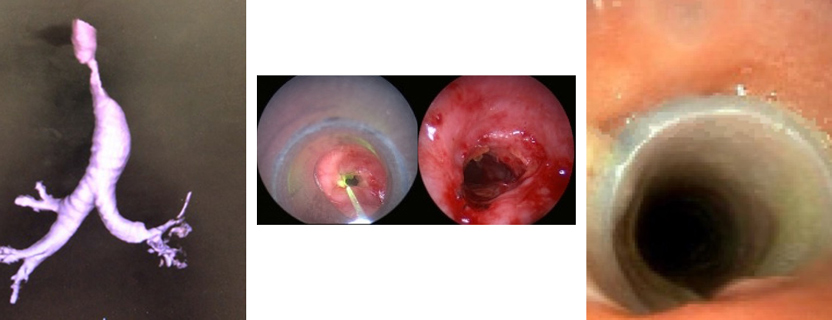
This procedure uses an indwelling laryngeal stent to improve the opening of the airway between the vocal cords in patients with posterior glottic stenosis.
Laser therapy uses ablation for tumoral tissues or precise scar tissue removal in benign airway stenosis. Laser therapy can be a standalone treatment or in combination with other techniques depending on the form of airway narrowing.
Laser Therapy Procedure Photos
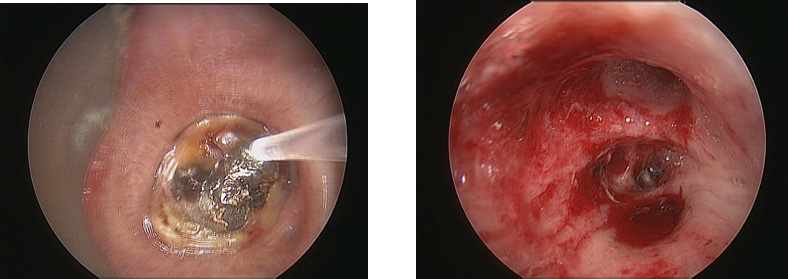
This procedure involves using a laser to remove the stenosis to improve airway size.
A variety of hot or cold therapies are used, such as electrocautery, argon plasma coagulation and cryotherapy are used to destroy scar tissue or tumor.
Photodynamic therapy, also known as light therapy, is a form of localized light-activated chemotherapy for inoperable airway tumors or for those with advanced cancers that cause airway blockages.
This procedure is used as an additional treatment for subglottic stenosis to decrease risk of recurrent symptoms.
Tracheal resection and reconstruction surgeries removes the affected airway segment and joins the airway back together. We perform laryngotracheal resection and reconstruction when the diseased airway segment is higher up in the neck and involves the cricoid cartilage. We also perform this surgery to treat tracheal stenosis and tracheal tumors.
Tracheal Resection and Reconstruction Surgery Photos
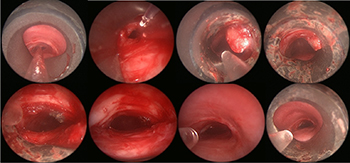
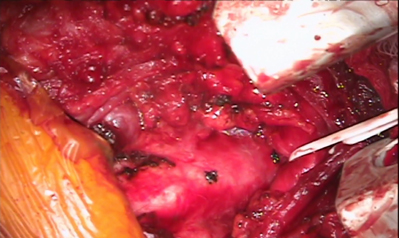
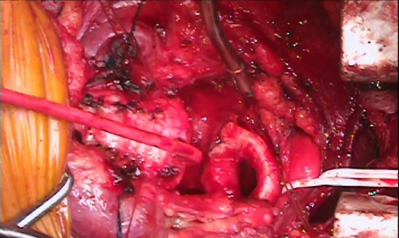
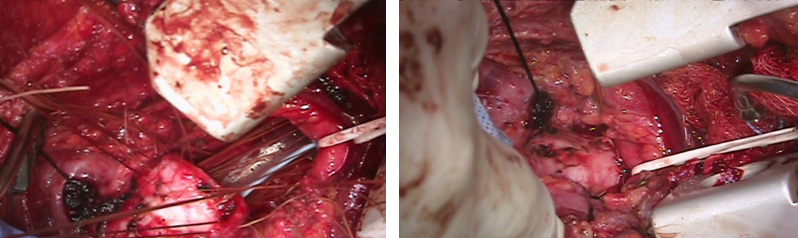
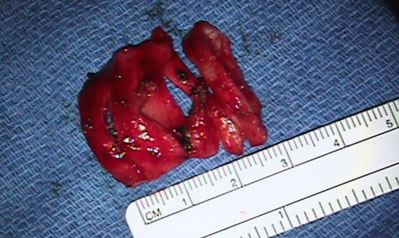
During tracheo-esophageal fistula surgery, the abnormal connection between the airway and the esophagus is repaired by suturing the defect closed and placing healthy tissue such as muscle in the repaired area.
Posterior tracheoplasty strengthens the back wall of the trachea with bioprosthetic materials for patients with tracheomalacia.
Our Complex Airway Disease Team
Request an Appointment
We are currently experiencing a high volume of inquiries, leading to delayed response times. For faster assistance, please call 1-773-702-1865 to schedule your appointment.
If you have symptoms of an urgent nature, please call your doctor or go to the emergency room immediately.
* Indicates required field






